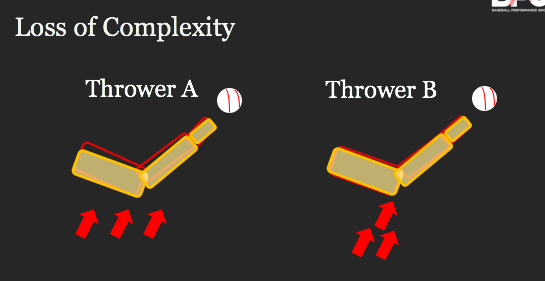
Why do I care so much about individual joint health? For the developing high school, college and young pro baseball player the primary focus is trending towards getting bigger, stronger, and throwing or hitting with weighted implements. We’ve seen an emergence of Instagram videos of pro pitchers benching big weight and articles on Thor squatting the house. It seems like everyone is throwing 95+, hitters are dropping mammoth blasts and here I am complaining that ‘joint health’ is being overlooked and under appreciated.
I’ve wrote about some of this stuff before on Baseball Think Tank and spoke about it at Palooza 16’, but I figured it would be worth divulging again. Hopefully I don’t muddy up the waters and leave you with an idea of how to assess articular health on a basic level.
Recently, I posted about the concept of hip dissociation on Instagram. In it, I discussed how we’ve been seeing a lot of pitchers with out-of-synch pelvis to upper trunk separation that we thought was linked to inadequate trail leg movement. Specifically, we noticed that these pitchers displayed an inability to independently rotate their femur relative to their acetabulum.
Their hip articulation, which is composed of the femur and acetabulum, was not functioning like a joint should.
When comparing our guys to elite MLB pitchers we noticed a stark difference between the two groups. While the Chapman’s of the world seem to move these components independently, our guys do not. It’s almost as if their trail leg femur and acetabulum were glued together in movement.

“A joint should act like a joint.”
We can argue all day about how much rotation is necessary for efficient kinematics in the trail hip (we believe a fair amount) but that is not the point here. If we take a pitcher, put them on a table and check their hip articulation, we should be able to see the femur move independent of the pelvis. What is commonly termed ‘dissociation’.
The ability to display articular dissociation isn’t limited to the hip joint but should be a trait seen throughout the body. Whether the movement we are trying to change involves hip rotation or glenohumeral flexion, we must have an idea of what the joint can handle. In other words, we should be asking ourselves “can your joints do what you’re asking them to do?”
Moreover, not only should we be able to see passive dissociation on a table but athletes should also be able to show active dissociation and articular independence. Players should be able to move their femur without moving their entire pelvis or the rest of their body!
HOW DOES THIS FIT INTO MOVEMENT, TRAINING AND INJURY?
The way in which movement emerges is a constantly evolving and dynamic process. When we first begin the solve a particular movement task, such as throwing a baseball, our body will try out a number of possible solutions. These solutions are influenced by the constraints placed on the system — things like the environment, the context of the task, the person themselves and a myriad of other factors. Over time and thousands of repetitions, many different solutions will be felt out until the body settles into a preferred pattern of movement.

This movement pattern will settle on certain parameters for stability — what are called attractor states. The stability of these attractor states will be determined by the number of repetitions, the context and variance of the learning environment, the task, etc and is, again, a constantly evolving process. With every repetition that pattern is being influenced or sculpted. To go along with these attractors, movement patterns will also display fluctuators. That is, components of the pattern that are flexible and able to adapt to the changes in the task dynamics.
With every repetition of the intended task – for example throwing a fastball up and in – there will be variations to the constraints placed on the movement system. Let’s remember for a second that constraints can be categorized as environmental, organismic, and task related. The wind may be stronger, there may be a lefty in the box instead of a righty, or the pitcher may be fatigued versus fresh. The conditions for the task (and the task itself) will never be the same.
When a change in constraints occurs the stability of the movement pattern is endangered. Whether or not we knock the attractor state out of it’s well and alter our movement will be influenced by the variance in constraints.
Let’s put this together with a common scenario.
A pitcher begins the off-season addressing the movement or joint limitations incurred from the long season. They spend their time restoring ‘normal for them’ glenohumeral, elbow and hip arthrokinematics. Over the rest of the offseason they make sure to maintain controllable range while gaining strength and hypertrophy in the gym and improving efficiency on the mound.
As the season progresses, the pitcher maintains his strength & power but places much less emphasis on maintaining range of motion. Although it seems like their mechanical changes are holding up, they unknowingly begin to lose small amounts of shoulder internal rotation, elbow supination and lead leg internal rotation. The stability of the movement pattern is being tested by these altered constraints until one day it eventually changes. New areas of the body seen acute spikes in stress and demand; too much and too quick relative to what they’re used to. A few weeks go by with increased soreness and then one day it becomes too much to bare. Pitcher goes on the DL.
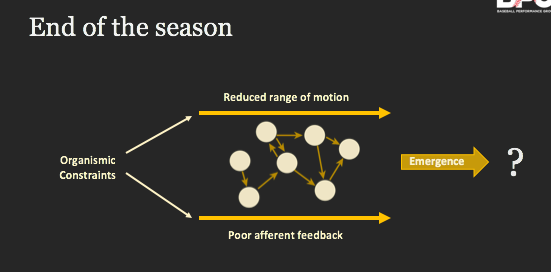
We lose degrees of freedom throughout the season
How about another scenario
A professional pitcher goes into the off-season looking to put on a lot of strength and size with the thought that it will gain him a few extra clicks and more mileage for the season. Everything goes according to plan; he gains 10 lbs, his lifts go up and he heads into spring training feeling stronger and more jacked than ever. He wasn’t really paying attention to how much controllable range of motion he lost this offseason but he only feels slightly tighter. As spring training progresses and he is asked to solve the ‘pitching task’ with more frequency, the (organismic) constraints on his system have changed as compared to last year. He now has less options to solve the task and his solutions, therefore, become more rigid and inflexible.
As the task become more and more frequent, and the variability of which he can solve the task is diminished, the same areas keep getting loaded. Where variability in the past may have served him well, rigidity in the present contributes to more consistent loading to a particular area. The process continues on for a few weeks until the inevitable happens — a particular tissue is asked to bear too much demand relative to it’s capacity and a tissue strain occurs.

A loss of co-ordinative variability may result in increase repetitive loading.
Navigating a constantly dynamic and variable environment requires the ability to be both stable and adaptable. Athletes must be able to express flexibility (but not too much) in their coordination and require options to do so. My thought process, at least for right now, is that we want to provide options for movement in the form of well articulating joints and maintain constraints within a range of tolerance that will not destabilize a movement pattern. Especially when it comes to large, repetitive workloads.
As we accumulate innings throughout the season, our goal, therefore, is to maintain a pattern of movement (for which we’ve built up tissue capacity) and promote flexibility within that pattern.
WHY CARE SO MUCH ABOUT JOINT MOVEMENT?
How we co-ordinate movement is a deeply complex subject. The interactions between all of the components of the movement system — joints, tissue, thoughts, emotions, environmental changes, perceptual changes, etc — are far too complex to extrapolate with any sort of certainty in injury (at least in my opinion, anyways). We could attempt to account for all of these constraint changes, their interactions with each other and how they ultimately affect the movement system but it’s probably too difficult of a task.
I think it makes much more sense to control for what we can (kinda) control for — useable range of motion and joint dissociation.
If we know that a movement pattern will be endangered via constraint changes, and range of motion is a significant organismic constraint that we can reasonably keep track of, then maybe we should pay more attention to it.
HOW WE KEEP TRACK OF THEM
Each of our athletes goes through a comprehensive assessment as part of the on-boarding process. During that time, we look at each individual articulation for passive dissociation, active dissociation and full controllable range of motion. This information is collected on paper and video, uploaded for each athlete online and can then used as a baseline for future reference. Throughout the training process, we perform check-ins to see how their movement is evolving, make alterations to their program and attempt to identify issues before they come up.
Not every program has the ability to perform “articular check-ins” with a full check of passive and active range, so we need something that will allow players to be self-sufficient.
CONTROLLED ARTICULAR ROTATIONS
Taken from the Functional Anatomy Seminars group, Controlled Articular Rotations (CARs) are an excellent tool for diagnosis of articular limitations. Performing them is a relatively straightforward process, doesn’t require fancy measurement tools, and can provide valuable information about the health of a joint.
We use them as a means to check for abnormal joint function (in the form of a pinching pain), to explore and account for changing outer ranges of motion and as part of our warm-up. CARs provide information that can be invaluable for a therapist, like position of provocation, and promote self-direction for what needs to be improved.
Active, rotational movements at the outer limits of articular motion.
Simple, huh? Our goal is to take our joints through as big of a rotational range of motion as possible without moving anywhere else in our body. In order to aid in that process, and keep things that aren’t supposed to move in place, we can use varying irradiation techniques. For a joint screen, however, we keep it simple by simply trapping air in the lower abdomen.
General rules for CARs.
- Inhale, trap air in lower abdominal region for irradiation.
- Stabilize all articulations in order to minimize extraneous movement.
- Be slow and smooth as you take rotate through the outer limit of movement.
- Attempt to expand the circle with each rep.
The goal is to perform around three repetitions per articulation in each direction. The level of tension that we are bringing into these movements is low, so don’t worry too much about co-contracting the house with movement.
We ask our athletes to go through every articulation in the body, but I will provide the main four below.
Glenohumeral Joint
Elbow Joint
Hip Joint
Spine – Cat / Camel
Our athletes are encouraged to perform these CARs every single day in the morning. In doing so, they are maintaining range of motion that they have, they are breaking down tissue fibrosis and stimulating regeneration from the day prior, they are developing a feel for what’s ‘normal’, what’s changing, and what needs a therapeutic input.
If a specific range is getting progressively smaller then that is information that I want to know. I want to know that before they start developing pain and discomfort. I want to account for any changes in the individual components that make up the human movement system. Maybe it’s something that they can address individually without seeing me. Our guys have a feel for this.
It’s easy. It’s free. It should be incorporated tomorrow. If you want to learn more about articular health and see more videos on mobility you can follow us here.
