Humeral Retrotorsion Part 2: Implications to Shoulder Health and Practical Applications
by Ryan Faubert | Sept 15th, 2022
This post is a continuation of Humeral Retrotorsion Part 1: At What Age Should Athletes Begin Throwing?
Introduction
It’s great that you decided to continue with part 2, because it digs a little further into some of the concepts discussed in part 1 with a hint of practical knowledge that you can implement in your practice, facility and/or athletes right away.
Let’s kick start this article by diving into why Humeral Retrotorsion is good for shoulder health in baseball players.
Why do we Care About External Rotation?
Static shoulder range of motion restrictions are believed to be a good predictor of injury in throwing athletes. A recent systematic review done by Trasolini et al. (2022), found that athletes with preseason external rotation limitations, which were only <5° greater than their non-throwing arms, had an increased risk of injury at about 1.9x.
The mechanism behind this is that the athletes need to be able to reach maximal external rotation that matches their late cocking phase angle passively to protect shoulder health.
Theoretically, this is thought to decrease the load on the surrounding soft tissue within the glenohumeral joint and the anterior capsule of the shoulder. Conversely, if the shoulder cannot get into optimal external rotation the anterior capsule and surrounding soft tissue structures will be challenged in a more lengthened position, which is a possible mechanism of increased injury. Hence if the athlete can reach optimal positioning it is thought to decrease tensile forces on the soft-tissue structures in the shoulder which includes the long head of the biceps and the rotator cuff tendons as well as the labrum.
Noonan et al. (2015) also found that athletes with decreased HR had a significantly increased risk of shoulder injury. This is due to the shoulder experiencing less external rotation since the humerus is already pre-oriented in an externally biased position at rest. As the shoulder is already pre-oriented in an externally rotated position at rest it requires less motion to reach the late cocking phase while pitching.
In order to see this in players, you need to actually test external rotation and internal rotation.
Their total range of motion from internal to external rotation should have approximately 180 degrees of motion, however, internal rotation will usually be decreased to accommodate the increase in external rotation. This compensatory decrease in internal rotation is a phenomenon known as glenohumeral internal rotation deficit (GIRD). For example, instead of having 90 degrees of internal and external rotation, you will have around 60 degrees internal and 120 degrees external.
Figure 1 below is a sample shoulder range of motion assessment on one of our athletes at the facility.
How to Test and Calculate this Yourself
You want to first measure the athlete’s shoulder internal (IR) and external rotation (ER) with 90° of shoulder abduction (think arm raised so humerus is parallel to the ground).
- Then assess how many degrees of ER and IR that they can do passively.
- To figure out the total range of motion (total arc) as explained above – add these two numbers.
- You want to compare this to their non-dominant arm to get a sense of ‘normal’ for the athlete as this can be variable.
- Then you will be able to use the difference in ER and IR to figure out approximately how much HR that an athlete has.
Let’s add some sample objective measurements from this and see how much HR the athlete below is displaying.
Calculation Example:
We have an athlete that has the following ranges of motion
- Dominant (top two images): ER= 120°, IR = 60°
o Total Range of Motion = ER+IR, which is 180°
- Non- Dominant (bottom two images): ER = 100°, IR = 80°
o Total Range of Motion = 180°

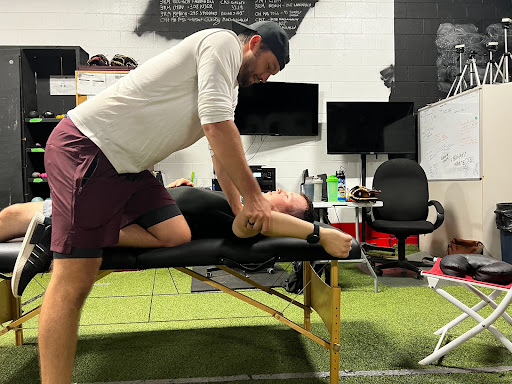
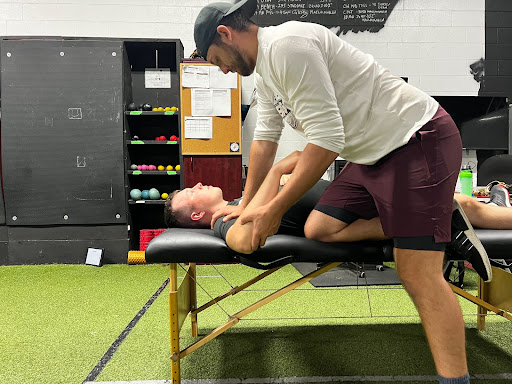
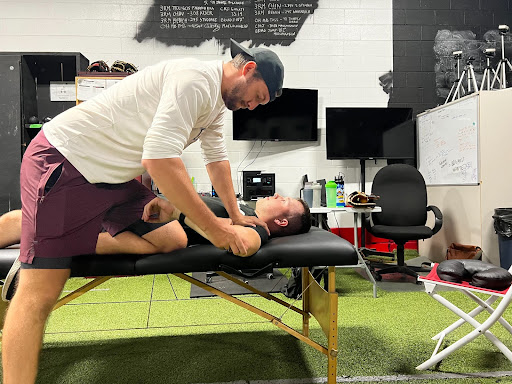
Figure 1: The top two images are illustrating ER and IR of this athlete’s throwing arm and the bottom two images are ranges of his non-dominant arm
Finding HR from this example is simply comparing the difference of ER and IR in both shoulders. As you can see there is a 20° gain of ER and a 20° loss of IR in the dominant shoulder. Therefore, we can conclude that this athlete is experiencing approximately 20° of HR in his dominant shoulder.
Why Do We Care?
Before I talk about this we need to know how to differentiate between pathological GIRD and anatomical GIRD. Every overhead athlete will probably demonstrate some sort of GIRD. Is this due to anatomical adaptation (change in bony anatomy) or is it a pathological finding that we need to investigate more? Anatomical GIRD will present as a shift in the total range of motion explained above. This means that both shoulders will have the same total arc motion (internal rotation + external rotation) but the throwing shoulder will just be shifted into having more external rotation and less internal rotation.
So there still may be a 20-degree difference in internal rotation but as long as the total arc motion is close, it is OK.
However, pathological GIRD is when there is a loss of total arc range of motion within the throwing shoulder and also an internal rotation deficit of over 20 degrees. This can put stress on the soft tissues surrounding the shoulder joint. This is because they need to compensate for this loss of total arc motion in order to accelerate the baseball.
Now that you understand what HR looks like, how to best assess it, and the difference between types of GIRD, it’s time to dive into some of the benefits this information gives us. As we saw above, with an increase in external rotation there should be a compensatory decrease in internal rotation.
How Much IR Lose is worth our Concern?
A study done by Lin et al. (2020) defined GIRD as a 20-degree deficit of IR when comparing the dominant arm to the non-dominant arm, assessed using the same method above. As you can see the athlete in the example above is showing objective findings of GIRD.
What does this mean for an athlete?
Following this further, the same study as above compared non-GIRD and GIRD baseball players. The players with GIRD had a correlated increased risk of injury. This study summed this up by stating that:
“GIRD pitchers fail to properly transfer power from the trunk to the throwing arm, and thus rely more heavily on the shoulder joint during pitching”.
They concluded that it was due to the “modified pitching mechanism” of baseball players with GIRD that had caused an increased risk of injury. Additional recent research has high quality evidence to show that deficits in total arc motion and IR were associated with increased upper extremity injury risk in baseball players.
Velocity is highly dependent on maximal humeral internal rotation angular velocity, built up during the acceleration phase of throwing. This is greatly dictated by the total arc motion.
For example, a pitcher who is throwing 90mph on average will usually exceed approximately 7000 – 7500 degrees/sec of internal rotation angular velocity (though it depends on the motion capture medium used).
That is fast.
If the shoulder has a loss in internal rotation and total arc motion, it can lead to excessive external rotation as a compensatory mechanism that can in theory cause injury to the posterosuperior structures like the labrum, possible cause of shoulder impingement, and leaving the elbow at risk for injury as well.
To support this, there was a systematic review and meta-analysis done in 2020 by Helmkamp et al., looking at “the relationship between HR and arm injury in baseball players”. A total of 2961 baseball players that were about 20.2 years +/- 12.3 years that were involved in 32 different studies were evaluated for this paper. Researchers demonstrated that internal rotation was affected by the degree of HR and decreased even more after pitching. They found that internal rotation deficits of the humerus was an amenable risk factor for injury.
Based on these points there are enough reasons to check this periodically in your athletes when the time is necessary to do so. Possible upsides to this include mitigation of shoulder injury risk and maintenance of shoulder health by being proactive in combating pathological GIRD. As coaches and trainers, we must take immediate steps to combat pathological GIRD and deficits in total arc motion to help mitigate the risk of shoulder injury.
This can include stretches, exercises, and/ or seeking professional care to be proactive before potential injury.
How Much IR Lose is worth our Concern?
Throughout this article, we found that the most effective way to gain external rotation is to throw. We also know that the optimal time to start throwing is approximately between the ages of 8-16 years of age. This is because on average at 16 years of age growth plates begin to fuse and adaptations are more difficult to come about in this time period. If you compare a 20-year-old to someone who is 14 there is a vast difference in bone formation and adaptation. In young adolescents, there is an ongoing process known as “peak velocity” aka puberty. This is the fastest and most adaptable time in their life that is influenced by increased hormone levels and its drastic effect on bone and muscle growth.
However, every child is different and can hit peak velocity at different times.
Theoretically, it would be correct to say that late bloomers picking up a baseball in high school for the first time would still be able to gain the adaptations needed to compete in baseball.
Situations like this have many variables but tentatively, skeletal maturity concludes when the growth plates close, which happens on average at age 25. Therefore, the most adaptable time can be within an 8-16 age range but adaptations to some extent can still occur until the later stages of skeletal maturity at 25.
An honourable mention goes out to weekend warriors who are either picking up a baseball for the first time or who already have a history of playing baseball.
As people age, their external rotation tends to decrease due to disuse, regardless of their baseball background. As a result of the cessation of motion, some ex-players have the humeral adaptation but a tightened shoulder capsule. Since the human body is highly adaptable, it tends to adapt when a stimulus is stopped or added. The shoulder girdle in general should be strengthened by athletes who fall into this category. We should also work on utilizing our range of motion through mobility exercises.
To withstand the forces placed on them during a pitching motion, people who are inexperienced with throwing and returning throwers will have to prepare their shoulders. Because of this, we need to strengthen the shoulder throughout the required full range of motion. More specifically focusing on passive and active ranges of motion in shoulder ER, IR, abduction, and flexion; and comparing possible deficits to the non-dominant shoulder. This way you can individualize your needs assessment and customize a plan of action to get ready for the upcoming season.
If possible, consider adding a build-up phase pre-season to get your shoulder used to throwing before trying to reach max-effort after taking a few months off. Although we may not gain HR in our later years, we can still benefit from soft tissue adaptations to compensate and allow us to participate in the sport we all love. Crucial components of build-up phases are improving mobility, strengthening, and increasing throwing volume and intensity gradually.
We need to prepare the shoulder to throw by releasing restrictions and gaining control. Once we have this you can load that shoulder joint as well as the rest of the body through the ranges of motions necessary to throw a baseball. Progressing with throwing starting from a light effort gradually increasing to high effort can set an athlete up for a successful segway into a baseball season. Such a build-up phase is necessary for most starting new activities, whether it’s baseball, softball, basketball, sprinting etc., in order to feel your best and enjoy yourself.
Even if we have previously attained the adaptations necessary to compete in said activities (or currently have them), after sustained time off from any sport we need to integrate the respective sports movement slowly, then gradually ramp up to high effort.
In doing so this will help to avoid injury and help you dominate in your league.
If you made it this far, thanks for reading this 2 part series on humeral retrotorsion. Hopefully you’ve learned something useful that you can share and apply with your athletes. If you have any questions feel free to reach out!
References
- Papas AM, Zawacki RM, Sullivans TJ. Biomechanics of baseball pitching. Am. J. Sports Med. 1985;13:216-22.
- Whiteley R. Baseball throwing mechanics as they relate to pathology and performance-a review. Journal of sports science & medicine. 2007 Mar;6(1):1.
- Seroyer ST, Nho SJ, Bach BR, Bush-Joseph CA, Nicholson GP, Romeo AA. The kinetic chain in overhand pitching: its potential role for performance enhancement and injury prevention. Sports health. 2010 Mar;2(2):135-46.
- Greenberg EM, Fernandez-Fernandez A, Lawrence JT, McClure P. The development of humeral retrotorsion and its relationship to throwing sports. Sports Health. 2015 Nov;7(6):489-96.
- Kay J, Kirsch JM, Bakshi N, Ekhtiari S, Horner N, Gichuru M, Alolabi B, Khan M, Bedi A. Humeral retroversion and capsule thickening in the overhead throwing athlete: a systematic review. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2018 Apr 1;34(4):1308-18.
- Greenberg EM, Lawrence JT, Fernandez-Fernandez A, McClure P. Humeral retrotorsion and glenohumeral motion in youth baseball players compared with age-matched nonthrowing athletes. The American journal of sports medicine. 2017 Feb;45(2):454-61
- Dwelley PM, Tripp BL, Tripp PA, Eberman LE, Gorin S. Glenohumeral rotation range of motion in collegiate overhead-throwing athletes during an athletic season. Journal of Athletic Training. 2009 Nov;44(6):611-6.
- Takenaga T, Goto H, Tsuchiya A, Yoshida M, Fukuyoshi M, Nakagawa H, Takeuchi S, Takaba K, Sugimoto K. Relationship between bilateral humeral retroversion angle and starting baseball age in skeletally mature baseball players-existence of watershed age. J Shoulder Elbow Surg. 2019 May;28(5):847-853. doi: 10.1016/j.jse.2018.10.017. Epub 2019 Jan 24. PMID: 30685277.
- Trasolini NA, Nicholson KF, Mylott J, Bullock GS, Hulburt TC, Waterman BR. Biomechanical analysis of the throwing athlete and its impact on return to sport. Arthroscopy, sports medicine, and rehabilitation. 2022 Jan 1;4(1):e83-91.
- Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder: spectrum of pathology Part I: pathoanatomy and biomechanics. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2003 Apr 1;19(4):404-20.
- Noonan TJ, Thigpen CA, Bailey LB, Wyland DJ, Kissenberth M, Hawkins RJ, Shanley E. Humeral torsion as a risk factor for shoulder and elbow injury in professional baseball pitchers. The American Journal of Sports Medicine. 2016 Sep;44(9):2214-9.
- Lin HT, Lin YC, Chou YL, Wu HC, Wang RT, Chou PP. Effect of Glenohumeral internal rotation deficit on shoulder in baseball pitchers during fastball pitching. International Journal of Environmental Research and Public Health. 2020 Nov;17(21):8211.
- Bullock GS, Faherty MS, Ledbetter L, Thigpen CA, Sell TC. Shoulder range of motion and baseball arm injuries: a systematic review and meta-analysis. Journal of Athletic Training. 2018 Dec;53(12):1190-9.
- Lin DJ, Wong TT, Kazam JK. Shoulder Injuries in the Overhead-Throwing Athlete: Epidemiology, Mechanisms of Injury, and Imaging Findings. Radiology. 2018 Feb;286(2):370-387. doi: 10.1148/radiol.2017170481. PMID: 29356641.
- Diffendaffer AZ, Bagwell MS, Fleisig GS, Yanagita Y, Stewart M, Cain Jr EL, Dugas JR, Wilk KE. The Clinician’s Guide to Baseball Pitching Biomechanics. Sports Health. 2022 Apr 23:19417381221078537.
- Helmkamp JK, Bullock GS, Rao A, Shanley E, Thigpen C, Garrigues GE. The relationship between humeral torsion and arm injury in baseball players: A systematic review and meta-analysis. Sports health. 2020 Mar;12(2):132-8.
- Cech D, Martin S. Functional movement development across the life span. 3rd ed. St. Louis: Saunders; 2012.

whoah this weblog is wonddrful i loive reding your articles.
Stay uup thhe ggood work! Yoou recognize, manhy people
arre looking arond forr thos info, you ccan aaid thrm greatly.